What is Obesity and Overweight?
What is obesity and how does it compare to what is overweight for an individual? At times, people use these two terms interchangeably, but they have distinct meanings. Individuals with higher BMI weigh more than is ideal or normal for their frame. And gender has greater body fat percentages.
An individual with higher BMI, have an excessive buildup of body fat that starts to affect their physical health. By harming their internal organs, joints, muscles, and other areas of their body. When a person weighs over 100 pounds or when major health issues. As conditions like type 2 diabetes, and high blood pressure start to manifest, doctors apply the phrase “class III obesity.”
Current Statistics, Trends
Over the past 20 years, the obesity rate in the United States has continuously increased. According to the CDC, class III obesity, formerly known as morbid obesity. It has doubled while the obesity rate among adults has increased from 30.5% to 42.4%. Childhood obesity has significantly increased. While it may be true, 20% or more of children between the ages of 2 and 19. Now categorized as individuals with higher BMI.
The second biggest preventable cause of premature death is obesity. Linked to depression, diabetes, arthritis, sleep apnea, heart disease, liver disease, and stroke.
How do we determine obesity, and what weight do we consider extreme?
Because each person’s build differs, we cannot accurately define exactly what weight we consider extreme. Therefore, what one person considers extreme may not be the same for another. Doctors consider an individual who is 6’1″ and weighs 175 pounds to be of a healthy weight. But they consider someone who is 5’1″ and weighs 175 pounds to have a higher BMI.
The majority of medical practitioners utilize the BMI scale, or body mass index, as a simple method to identify obesity. Even though it cannot accurately determine a person’s health or detect their body fat percentage. But it can easily categorize them based on their weight and height. A number of these categories signal that a person’s weight may result in serious health problems.
The Standard BMI Scale
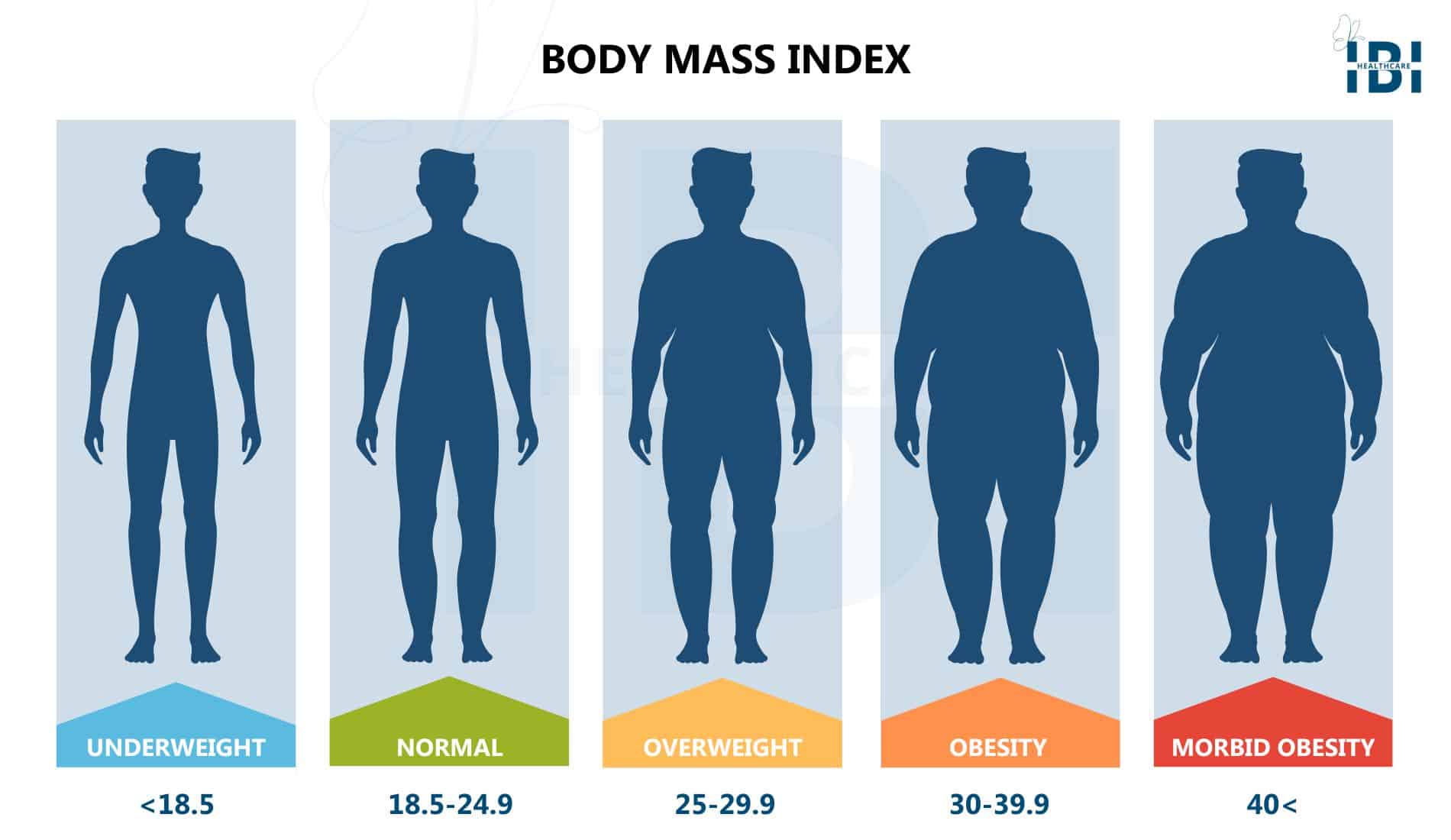
- Underweight – Less than 18.5.
- Healthy weight – 18.5 to 24.9.
- Overweight – 25 to 29.9.
- Class I Obesity – 30 to 34.9.
- Class II Obesity – 35 to 39.9.
- Class III Obesity – 40 to 49.9.
The BMI scale is not perfect. It does not account for variances. Like trying to separate muscle mass from fat mass when determining obesity. According to the BMI calculator, it categorizes the majority of NFL football players as extreme. Although this is untrue. It merely serves as a quick, simple, and affordable method of aiding in the categorization of people into weight classes. But it has limitations. You can check your BMI below. And get a quick idea of where your current weight falls.
Obesity and Overweight - Causes and Consequences
We still do not fully understand obesity, which is a complex condition. Individuals with higher BMI retain more fat than they burn. Sometimes, it’s easy to explain why some people store or burn more fat than others under similar conditions. While other times, it can be more complicated.
Poor lifestyle choices such as overeating, and consuming unhealthy meals. Alongside, lack of exercise all contribute to weight gain. However, other less evident underlying variables might contribute to weight gain. Such as genetics, hormonal imbalances, and regional or economic impacts. Cultural variations, environmental factors, drugs, stress, psychological disorders, and metabolic abnormalities are a few common contributors.

Obesity and Overweight - Causes
1. Behavior and Lifestyle Choices
Healthy eating habits and consistent exercise are examples of healthy practices. To keep from gaining too much weight, we need to keep a balance. The calories we eat and the calories our bodies need to function.
The expert-recommended Dietary Guidelines for Americans emphasize. Eating whole grains, vegetables, fruits, lean protein, low-fat, and fat-free dairy products. Additionally, drinking water is the foundation of a healthy dietary plan.
Besides the healthy diet, according to the Physical Activity Guidelines for Americans. Adults should do at least 150 minutes of moderate-intensity activity. 75 minutes of vigorous-intensity activity, or a mix of the two each week. They should also do two sessions of strength training.
2. Community and Environment
Individuals may base lifestyle decisions on their surroundings or neighborhood. For example, if there is a lack of sidewalks or safe bike paths. A person might decide not to cycle or walk to the store or to work. People’s surroundings at work, home, daycare, school, and other places. Often influence their daily behaviors. Because of this, it’s critical to design environments in these places. That makes it simpler to engage in physical exercise and consume a nutritious diet.
3. Genetics
Currently, we understand that genetics can increase a person’s risk of developing obesity by up to 70%. There are more than one hundred genes and variations associated with obesity. The fact that inherited obesity risk does not necessarily translate into real obesity development. However, raises questions about the intricate relationships between genetic, behavioral, and environmental factors that contribute to obesity.
4. Medical Conditions and Medications
Some individuals with obesity may have a medical disease, such as Cushing syndrome, Prader-Willi syndrome, or another ailment. Reduced exercise might arise from medical issues like arthritis, which can also contribute to weight gain.
Weight gain may also be a side effect of various prescription drugs and medications. For instance steroids, some illegal substances, and antidepressants. A doctor with expertise in managing obesity can help identify potential medical issues. In fact, health concerns you may be experiencing may determine certain habits, conditions, and drugs. Furthermore, psychological issues are causing you to gain weight or are inhibiting your weight loss efforts.
Obesity and Overweight - Consequences
1. Health Consequences
Individuals with higher weights face a greater risk of numerous serious illnesses and health conditions. Compared to those within a healthy weight range, including the following:
- Stroke.
- Heart Disease.
- Type II Diabetes.
- Gallbladder Issues.
- Body and Joint Pain.
- Chronic Sleep Apnea.
- Decreased Quality of Life.
- Osteoarthritis – Joint Degeneration.
- Approximately 13 Different Cancers.
- High Blood Pressure (Hypertension).
- High or Low Cholesterol or Triglycerides.
- Depression, Anxiety, and Other Psychological Disorders.
2. Economic Consequences
Obesity significantly impacts the U.S. healthcare system financially. Additionally, obesity-related health issues cause both direct and indirect impacts on medical expenses. Direct medical costs may include preventive, diagnostic, and interventional treatments for obesity. Indirect costs include expenses such as lost productivity due to mortality and morbidity.
Premature mortality and disability are productivity measurements. As well as “absenteeism” related to costs associated with employees missing work. They are attributable to health issues created by their unhealthy weight. But also decreased productivity of at-work employees.
3. National Estimated Costs of Obesity
In 2019, the annual cost of medical care associated with obesity. It was close to 173 billion dollars in the United States. The annual productivity implications of weight-related absenteeism in the United States range from $3.38 to 6.38 billion dollars.
Additionally, obesity affects recruiting within the military services, in addition to these expenses. Utilizing the information gathered from the National Health and Nutrition Examination Survey results. We calculated the proportion of the American population.
That is of military age and overweight. Relative to the standards for active duty enlistment set by the United States Army. In the years 2007-2008, the Army set enlistment limits for weight and body fat. During that time, 5.7 million men and 16.5 million women. Eligible for military duty exceeded those standards.





